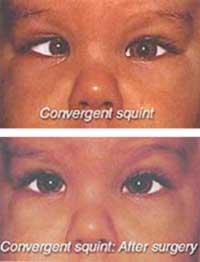
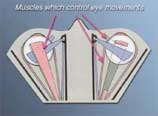
There are various types of ESOTROPIA (inward turning of eyes). Infants developing esotropia within the first three months of life (Congenital or Infantile Esotropia) usually have a large inward turn, which is easily noticed. The chances of developing normal binocular vision with normal depth perception are not good and may lose vision in the weaker eye. However, the best chance is with early aggressive surgery. Treatment after the age of 2 decreases the chances of improvement of vision, and the ability to use the two eyes together. Additionally, the cosmetic defect resulting from "crossed eyes" can have a negative effect on a child's self-confidence. Both the parent and surgeon have to be committed to multiple procedures to obtain perfect alignment. The aim of eye surgery is to adjust the muscle tension on one or both eyes in order to pull the eyes straight. In surgery for esotropia, the tight inner muscles are placed further backward which weakens their pull and allows the eyes to move outward. Sometimes the outer muscles may be tightened by shortening the muscle length, which further pulls the eye outward.
Strabismus surgery is usually a safe and effective treatment, but is not a substitute for glasses or amblyopia therapy. During surgery, the eyeball is never removed from the socket. A small incision is made within the tissues covering the eye to allow access to the eye muscles. Selection of eye muscles to be operated upon depends upon the direction the eye is turning. Despite a thorough clinical evaluation and good surgical technique, the eyes may be closely aligned after surgery, but not perfect. In these cases, fine adjustment is dependent upon the coordination between the eye and the brain. Sometimes patients may require the use of prisms or glasses following eye muscle surgery. Over-corrections or under-corrections can occur and further surgery may be needed.
One or both eyes may be operated upon. General anesthesia is required in children. Some adults may prefer local anesthesia. Recovery time is rapid and the patient is usually able to return to normal activity within a few days. As with any surgery, eye muscle surgery has certain risks. There is a small risk of infection, bleeding, excessive scarring, and other rare complications, which can lead to loss of vision.
Another common form of esotropia that occurs in children usually after age two is caused by a need for glasses (accommodative esotropia). These children are farsighted (hypermetropia or plus power in spectacles). They have the ability to focus their eyes enough to adjust for the farsightedness, which allows them to see well for both distance and near. Some children excessively cross their eyes when they focus, which causes one eye to turn in. Wearing glasses equal in strength to their farsightedness reduces the need to focus and straightens their eyes. Sometimes the addition of bifocals is necessary to further reduce the need to focus when looking at objects up close. Occasionally, eye drops and special lenses, called prisms, can be used to help the eyes focus properly. Rarely, special eye exercises (orthoptics) are necessary to help older children control the eye misalignment.
Know More...
 Dr. Varshini Shanker
Dr. Varshini Shanker Dr. Manish Malhotra
Dr. Manish Malhotra Dr. Sumedha Sharma
Dr. Sumedha Sharma





 Call Now
Call Now Book an
Book an Chat
Chat