Uveitis is characterized by inflammation of the inner coats of the eye. Patients complain of pain, redness, and diminution of vision. Uveitis is often associated with diseases that affect the rest of the body. It is commonly associated with disorders such as Rheumatoid Arthritis and Sarcoidosis. Viral infections and Tuberculosis are also associated with Uveitis.
(For further information please refer to frequently asked questions)
Team for Uvea & Ocular Inflammation
-
Dr. Shishir Narain
Kailash Colony
-
Dr. Priyanka Gupta
Kailash Colony, Ghaziabad
-
Dr. Richa Pyare
Kailash Colony, Gurgaon, Ghaziabad
Frequently Asked Questions
Uveitis (pronounced U'VE-I'TIS) means "inflammation of the uveal tract", or the middle layer of the eye. It is an immunologically mediated reaction in the uveal tract leading to its inflammation. It is important to clarify that there is no infection in uveitis. Uveitis may be an isolated problem or may be associated with inflammation in other parts of the body. It may be a single episode in some patients while in others it may have a tendency to be chronic and recurrent. We therefore thoroughly investigate a patient of uveitis to find a possible cause for this inflammation and its prognosis. To understand about uveitis and its seriousness, it may also be helpful to know the basic anatomy of this tissue of the eye.
Know More...
The uvea contains many of the blood vessels, which nourish the eye. Inflammation of the uvea can affect the cornea, the retina, the sclera, and other vital parts of the eye. Since the uvea borders many important parts of the eye, inflammation of this layer may be sight threatening and more serious than the more common inflammations of the outer layers of the eye. Also, due to its rich blood supply, the uveal tract is a natural target for diseases originating in other parts of the body. Because the cornea is normally clear, signs of disease may be seen inside the eye, often before signs develop elsewhere in the body.
Know More...
When any part of the uvea becomes inflamed, the condition is labeled as uveitis. This may be further subdivided depending upon the exact structures involved in the inflammation. Thus, if only the iris is inflamed it is called Iritis. Similarly Cyclitis is inflammation of the ciliary body. Anterior uveitis or iridocyclitis is inflammation of both the iris and ciliary body. Choroiditis or posterior uveitis is inflammation of the choroid. Intermediate uveitis is inflammation of the middle part of the uvea and is commonly also referred to as pars planitis. If all structures (iris, ciliary body and choroid) are inflamed then it is called panuveitis. These are medical terms but are helpful for you to know.
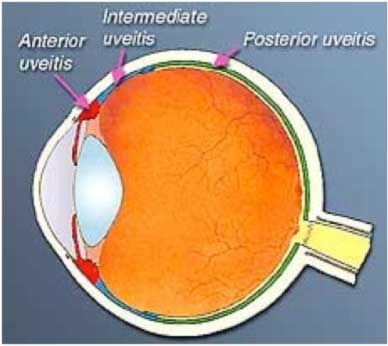
Know More...
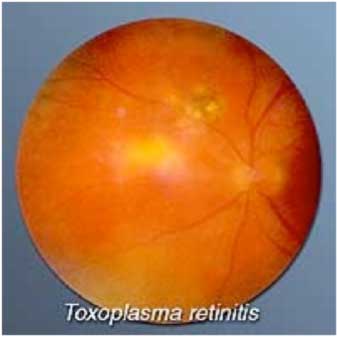
Uveitis results from a hypersensitivity to an external or internal protein; hence it may have many different causes. It may result from hypersensitivity to various infective organisms including viruses (such as shingles, mumps, or herpes), fungi (such as histoplasmosis), parasites (such as toxoplasmosis) and bacteria (such as tuberculosis, Lyme disease, and syphilis). It may be due to an underlying autoimmune disease. In the Indian scenario infectious causes account for a large proportion of uveitis cases.
Uveitis can also be related to disease in other parts of the body (such as sarcoidosis, arthritis & ankylosing spondylitis) or come as a consequence of injury to the eye. Rarely, inflammation in one eye can result from a severe injury to the fellow eye (sympathetic uveitis).
Additionally, uveitis may be caused if other structures of the eye are inflamed like a corneal ulcer or rarely a swollen hypermature cataract. In a few patients there may be genetic predisposition to inflammation that can be detected by HLA typing of your DNA in specific conditions. Despite thorough investigations, in a significant proportion of cases, the cause remains undetermined and is called idiopathic uveitis.
Know More...
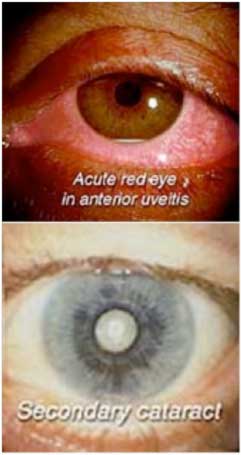
Depending on which part of the eye is inflamed in uveitis different combinations of symptoms may be present. These include redness of the eye, pain, light sensitivity, blurring of vision and floaters.
Uveitis may come on suddenly with redness and pain, or it may be slow in onset with little pain or redness, but gradual blurring of vision. These symptoms may also come on suddenly, and you may not experience any pain.
The symptoms described above may not necessarily mean that you have uveitis. However, if you experience one or more of these symptoms, contact your ophthalmologist (eye doctor) for a complete exam. Early detection and treatment is necessary, as inflammation inside the eye can permanently affect sight due to glaucoma (high pressure in the eye), cataract (clouding of the lens of the eye), or retinal damage, and rarely, lead to blindness.
Know More...
An ophthalmologist will use instruments to examine the inside of the eye and often can make a diagnosis on that basis. In some circumstances, blood tests, skin tests (Mantoux test), x-rays, and CT scans, and sometimes, even specimens taken surgically from the eye, may assist in establishing the diagnosis and finding its cause. Since uveitis can be associated with disease in some other part of the body, an evaluation and understanding of the patient's overall medical health is important. This may involve consultation with other medical specialists, including pulmonologists, immunologists or rheumatologists.
Know More...
The treatment of uveitis requires therapy to halt the inflammation of the uveal tract along with a search for the cause of the condition. Diagnostic tests may be needed to determine possible causes. The results of these tests are very important for proper treatment to be given. Medical treatment of uveitis must be aggressive to prevent glaucoma, to prevent scarring of the structures inside the eye and to prevent possible blindness.
Different medications are used to control the original cause of the uveitis, if detected, and to minimize the inflammation itself. Eye drops, especially steroids (to reduce inflammation and pain) and pupil dilators (to widen the pupil and relax the muscles within the eye), are the main medications used to treat uveitis. For deeper inflammation, oral medication or injections around the eye may be necessary, especially sub-Tenons' injection of depot steroids.
Sometimes if the inflammation is more prolonged or vision threatening then systemic steroids may be required. These drugs quickly control inflammation in a large proportion of patients. However, if used for longer periods these drugs cause weight gain and water retention, acne formation, osteoporosis and gastric ulcers, and require to be minimized during treatment.
Rarely if very prolonged systemic steroid treatment is required it may not be possible to do so because of the enumerated side effects. In such a situation, a patient may be switched over to special medicines called immunosuppressive agents. When given in low doses, these drugs decrease the number of white cells, which are the mediators of inflammation. These drugs, such as, Methotrexate, Azathioprine and Cellcept have different side effects including decreasing blood counts and mild liver and kidney dysfunction, which are partially reversible on stopping treatment. These can be detedcted by frequent blood tests and being under the care of a physician or immunologist.
Complications of uveitis such as glaucoma, cataracts, or new blood vessel formation (neovascularization), also may need treatment in the course of the disease. If complications are advanced, conventional surgery or laser surgery may be necessary.
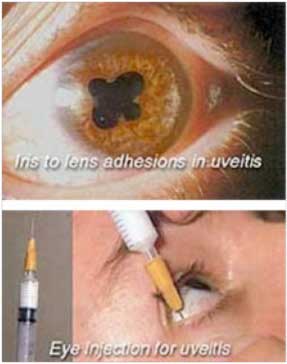
Know More...
Follow-up examinations ensure optimal therapy is being given and guard against possible complications. Uveitis, if caught early and treated diligently and appropriately, will often resolve without serious consequences.
Know More...
 Dr. Shishir Narain
Dr. Shishir Narain Dr. Priyanka Gupta
Dr. Priyanka Gupta Dr. Richa Pyare
Dr. Richa Pyare







 Call Now
Call Now Book an
Book an Chat
Chat