Team for Cornea
-
Dr. Rushad Shroff
Kailash Colony, Ghaziabad
-
Dr. Ritu Arora
Kailash Colony
-
Dr. Dariel Mathur
Kailash Colony, Connaught Place
-
Dr. Deepender Chauhan
Kailash Colony, Connaught Place, Ghaziabad
-
Dr. Amit Kumar Chawla
Kailash Colony, Gurgaon
-
Dr. Abhilasha Sanoria
Kailash Colony, Ghaziabad
Frequently Asked Questions
The eye is like a camera in which lenses focus the picture on a light sensitive film. In the human eye, the transparent cornea and lens focus light on the retina, which changes it into electrical signals. These signals are then transmitted to the brain by the optic nerve to be perceived as images.
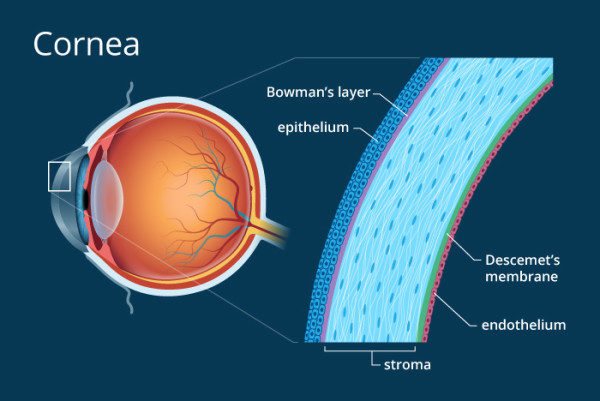
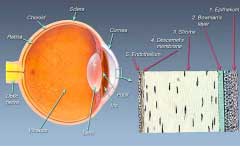 The cornea is the front transparent window of the eye. It is lamellar in nature (like plywood) and is made up of 5 layers, each of which has a definite function. In order to be effective it must remain transparent. Damage to any layers of cornea by degenerative change, infection, injury or scar tissue causes blurred vision due to loss of its transparency. Such a condition is called as corneal blindness.
The cornea is the front transparent window of the eye. It is lamellar in nature (like plywood) and is made up of 5 layers, each of which has a definite function. In order to be effective it must remain transparent. Damage to any layers of cornea by degenerative change, infection, injury or scar tissue causes blurred vision due to loss of its transparency. Such a condition is called as corneal blindness.
Know More...
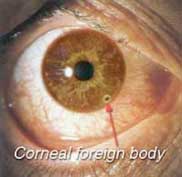
Since the abundant nerve supply of the cornea makes it one of the most sensitive parts of the body, it serves as an excellent "watchdog" for foreign material entering the eye. Dirt or specks lodging in the eye may produce scratching, knife-cutting sensations that the sensitive corneal nerves transmit to the brain. If the cornea loses this sensitivity due to in- jury or impairment by disease, it loses its protective function. Foreign bodies may embed in the cornea. A foreign body on the cornea needs urgent attention by an ophthalmologist. One should not attempt to remove it by rubbing the eye.
A twig of a tree, a piece of paper, or a fingernail can produce corneal abrasions. If not attended to immediately, secondary infection can occur which could lead to vision-threatening complications. Contact lenses also can produce an irritable eye from a corneal abrasion. Until an eye specialist can be consulted, the contact lens should be removed and the eye patched.
Injuries to the eye with sharp or blunt objects require urgent attention of your ophthalmologist, especially to rule out corneal injuries, which can be sight-threatening.

Know More...
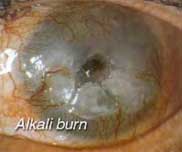
Acid or alkaline solutions splashed into the eye may be potentially sight threatening. Symptoms (such as pain, redness, watering and light-sensitivity) occur immediately after exposure to the chemical and may be severe in nature. Chemicals in the eye need to be thoroughly washed out immediately with water. THEREAFTER, URGENT CONSULTATION WITH AN EYE SPECIALIST IS NECESSARY.
Know More...
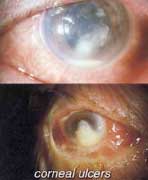
Inflammation of the cornea, or keratitis, may be secondary to conjunctivitis, blepharitis (inflammation of eyelid margins), or injury. Keratitis is characterized by a painful red eye, sensitivity to light, and an occasional scratching sensation upon blinking. An ulcer may develop in the cornea after a bacterial, viral, fungal, or other infectious organism invades its outer layer. Herpes simplex, a virus can invade the cornea after injury, producing keratitis. Herpes zoster, another viral agent, produces inflammation of the cornea, especially if the skin of the nose is involved. A marginal ulcer is a corneal infection that occurs near the outer edge of the cornea. Central corneal ulcers due to bacteria, viruses, or fungi can be severe and serious; they may even cause loss of the eye. With these severe ulcers, the eye sets up a defense reaction to help fight the infection. This disease requires the immediate attention of an ophthalmologist. With intensive medical treatment, the infection is brought under control. Sometimes drastic surgical intervention has to be undertaken. Often after elimination of the infection, there is residual scarring of the cornea, which requires corneal transplantation for restoration of vision.
Know More...
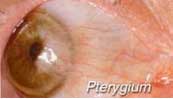
This grayish elevated growth of elastic and connective tissue containing blood vessels invades and grows over the cornea. It may result from irritation to the eye from wind, heat of the sun, dust, or smoke. If the pterygium progresses to grow over the center of the cornea, sight may be impaired or even lost. Before this occurs, the pterygium should be removed surgically. At our centre, pterygium is removed by a specialized technique called Conjunctival Autografting, where, the pterygium is excised, and a conjunctival graft, taken from a healthy part of the same eye is used to cover the defect. This technique prevents recurrence of the pterygium, which would normally occur after conventional pterygium removal without grafting. Some people confuse a cataract with a pterygium by calling a cataract a "skin growing over the eye." A cataract, however, is a clouding of the lens, which is located inside the eyeball.
Know More...
Dystrophies or degenerative aging processes may develop in the cornea and interfere with vision. They are slowly progressive, non-inflammatory, and usually affect or involve both eyes. They may produce a haziness or cloudiness of the cornea. If the vision is markedly impaired, contact lenses may be prescribed to improve vision. If they do not help, a corneal transplantation may be performed to restore useful sight.
Know More...
Dry eye syndrome is a leading cause of ocular discomfort affecting millions of people. Dry eye conditions are a spectrum of disorders with varied etiology ranging from mild eyestrain to very severe dry eyes with sight threatening complications.
Although the typical patient of dry eyes is elderly, or suffers from autoimmune disease, increasing numbers of patients do not fit this profile. Younger patients who work with computers can suffer from dry eyes more often than elderly patients. Dry eye condition is also aggravated in polluted conditions, dry weather, decreased ambient humidity as seen with air conditioning and indoor heaters. It may also result from the abnormalities in one or more of the tear film components, ocular or systemic diseases, and various drugs.
Dry eye syndrome is usually treated with tear supplements and lubricants. However, if these do not help, the insertion of microscopic plugs (temporary or permanent) can be inserted to help conserve tears and prevent them from draining away. In severe cases, surgical intervention may be essential.
Know More...
Normally the cornea is nearly spherically shaped thus allowing light to be focused clearly on the back of the eye (retina). However in a condition called Keratoconus, the cornea begins to thin, and this allows the normal pressure of the eye to make the cornea bulge forward taking on a cone-shape. As the cornea gradually becomes more cone-shaped, the vision blurs and becomes distorted due to a high degree of astigmatism. Initially vision may be correctable with spectacles, but as the condition progresses, and the cornea becomes more irregular causing distorted vision, spectacles become less effective. In such a situation, contact lenses not only provide better vision, but also help to retard the progress of the disorder. A rigid contact lens (RGP / "semi-soft" contact lenses) must be used, so that it can hold its shape, as a soft lens would simply mould to the existing shape and thus not allow complete correction of the problem. Sometimes the patient is fitted with soft lenses (for comfort), over which semi-soft lenses are fitted ("piggy-back" lenses).
Fitting contact lenses for keratoconus requires expertise. Well-fitting contact lenses dramatically improves such a patient's vision to nearly that of a normal person's, and significantly improves his or her quality of life. Any excessive pressure of a poorly fitting lens on the cone apex can cause permanent scarring within months or years (This scarring can also occur naturally). For this reason it is important for regular follow-up visits to be made so that any corneal changes that have occurred can be compensated for in the design of a new lens. It is quite common for patients to be refitted at irregular intervals as the condition progresses. Rarely, scarring is so severe that a corneal graft (transplant) is necessary.
A recent promising treatment modality for keratoconus is C3R (Corneal Collagen Cross-linking with Riboflavin). Shroff Eye Centre now offers you Cross Linking of the Cornea with Riboflavin (C3R), which is a new curative approach to increase the mechanical stability of corneal tissue. The aim of this treatment is to create additional chemical bonds inside the corneal stroma by means of a highly localized photo polymerization.
The indications for cross linking today are corneal ectasia the disorders such as keratoconus and pellucid marginal degeneration, iatrogenic keratectasia after refractive lamellar surgery and corneal melting that is not responding to conventional therapy.
Know More...
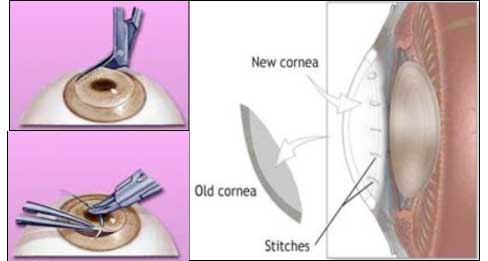
Corneal transplantation or keratoplasty is also known as corneal grafting. It is an operation designed to correct blindness resulting from corneal disease. It involves removal of the damaged or diseased cornea which is replaced by donated healthy corneal tissue (the graft) either in its entirety (penetrating keratoplasty) or in part (lamellar keratoplasty). The graft is taken from a recently deceased individual with no known diseases or other factors that may affect the viability of the donated corneal tissue or the health of the recipient.
Only the corneal tissue (and not the whole eye) donated by one person is transplanted into the diseased eye of another person who has been blinded by a corneal scar or disease.
Know More...
Some mistakenly believe that a blue-eyed person's eyes cannot be used for transplantation in a brown-eyed person. The only tissue used in the transplant is the cornea, which has nothing to do with the colored part of the eye.
Know More...
Many people are under the false impression that one good eyeball is transplanted for another eyeball which is diseased. Since the eye is connected to the brain by the optic nerve, which is a part of the central nervous system, the eye is not and cannot be transplanted.
Know More...
There is a perpetual shortage of donor corneas in our country due to poor awareness about eye donation. That’s why you need to first register for corneal transplant. The waiting period depends on the voluntary donation of eyes from the community.
A corneal transplantation, like a cataract operation, is usually performed under local anesthesia. General anesthesia is used for children and apprehensive or nervous patients. The operation is completely painless and takes about one hour to perform.
The diseased, cloudy, opaque cornea is removed from the recipient's (living patient's) eye using a special blade, and replaced by a new clear cornea (graft) from the donor's (deceased person's) eye. The new cornea is then sutured or stitched into place. Usually, 16 sutures are used to hold the graft or transplanted cornea in its position.
Recently, a new technology called Femtosecond Laser (IntraLaseTM) is available to make precise laser aided cuts in the donor and host cornea. Intralase-aided cuts improve wound healing and require less number of sutures leading to faster recovery.
Know More...
Corneal transplantation restores vision only in eyes that have been partially blinded by corneal disease. If a person is blinded by glaucoma, a detached retina, or degenerative change and the retina has been damaged or destroyed, nothing can restore lost sight.
In favorable subjects the rate of success of corneal transplantation may be as high as 90%, with good final visual acuity with glasses. In unfavorable subjects, the rate of success may be around 10 to 20%. Each patient is evaluated individually before definite results can be predicted. The most important factors in determining the final results are:
• Basic corneal disease (some types of corneal disease respond better to corneal transplantation than others).
• State of the donor's cornea.
• Surgical technique and skill.
• Healing ability of the recipient cornea.
• Sensitivity reactions between donor and recipient cornea may lead to transplant rejection.
• Presence of concurrent eye diseases like glaucoma, retinal diseases reduce the chances of good visual outcome
The advantages of lamellar keratoplasty (newer techniques) are better visual outcome, quicker rehabilitation and lower rates of transplant rejection.
Know More...
If the operation is successful and the graft is accepted by the recipient eye, it remains clear and the vision starts to improve with time (provided the lens and the retina behind the cloudy cornea are normal).
Healing after corneal transplant is a slow process and takes up to 1 year before all sutures can be removed. The vision fluctuates over the first 6 months and glasses are prescribed after healing is complete.
Additional surgery like LASIK or PRK can be done if patient wants to get rid of glasses.
Know More...
In conventional corneal transplant surgery (Penetrating Keratoplasty), the surgeon removes the window of cloudy tissue from patient’s cornea and replaces it with a clear corneal tissue. This transplanted cornea is held in its place with multiple tiny stitches. To allow healing, these stitches must remain in their place for at least 6 months. These stitches induce an irregular spectacle number (irregular astigmatism) in the eye and it takes long to get a clear vision.
DSEK and DSAEK is a selective keratoplasty in which only the diseased endothelial layer of cornea is replaced by a healthy donor tissue. The procedure requires precision guided dissection of donor tissue to retrieve only the innermost layers of cornea. This can be accomplished with an automated micro-keratome or by Femtosecond Laser (IntraLaseTM). As less tissue is transplanted, lower rejection rates may be expected, esp. epithelial and stromal rejection. DSEK/DSAEK procedure requires less number of sutures, it is safer and visual recovery is faster compared to conventional penetrating corneal transplant.
What happens if the graft fails?
Graft failure can occur due to infection, rejection or glaucoma. Should the graft fail, it can be replaced by a repeat corneal transplantation.
Know More...
The patient is usually hospitalized for one day but requires rest for the next one month although returning to light work is not a problem. However frequent follow-ups are required over the following six months to one year.
Meticulous post op care of the operated eye is required. Patient should maintain good hygiene, avoid rigorous physical activity and must not rub the operated eye.
THE OCCURRENCE OF PAIN, REDNESS, WATERING, LIGHT-SENSITIVITY AND DIMINISHED VISION, ANY TIME (EVEN MONTHS OR YEARS) AFTER CORNEAL TRANSPLANTATION SURGERY, REQUIRES IMMEDIATE ATTENTION OF YOUR OPHTHALMOLOGIST.
Know More...
Patient’s immune system can identify the transplanted cornea and mount a reaction against it. As a natural phenomenon, any organ transplant carries a risk of rejection. A severe rejection episode can cause irreversible loss of function and graft fails. However, recognizing early warning signs of rejection and a regular follow-up can prevent graft failure due to rejection. This is why a regular and long-term follow up is required after corneal transplant.
Corneal transplant is a human effort to match what nature has created. Many factors like graft rejection, infection, astigmatism and glaucoma limit the ultimate success of corneal grafting. Despite many limitations, corneal transplant is still the most successful story among all organ transplant procedures.
Endothelial Keratoplasty / Descemet’s Stripping Automated Endothelial Keratoplasty (DSAEK)
Introduction:
Corneal endothelium is the innermost layer of cornea. It comprises of a layer of endothelial cells lined by a thin transparent membrane (Descemet’s membrane). The endothelial cells maintain corneal transparency by pumping excessive water from the corneal tissue. Any injury to endothelial cells is permanent as theses cells can not divide and grow once damaged.
Corneal endothelial disorders like pseudophakic bullous keratopathy (clouding of cornea after cataract surgery) and Fuchs’ endothelial dystrophy (clouding of cornea as a result of inherent corneal disease) are one of the major indications of corneal transplantation. Ideally, the corneal endothelium is the only layer that requires transplantation in these conditions, thus making endothelial transplantation as the treatment of choice. However, still majority of these cases undergo full thickness penetrating keratoplasty, which is often complicated by high irregular astigmatism (cylindrical number), a weak host graft junction due to slow wound healing, suture related infections and corneal graft rejection. Many of these complications can be avoided by a sutureless selective corneal endothelial transplantation technique. Descemet Stripping Endothelial Keratoplasty (DSEK) and its variations like Descemet’s Stripping Automated Endothelial Keratoplasty (DSAEK) and Femtosecond Laser assisted DSAEK are modifications of endothelial keratoplasty. The fixation mechanism is so effective that sutures are not required. The posterior transplant consists of the endothelium, DM, and a thin layer of posterior stroma. It stays apposed to posterior corneal surface due to the negative pressure induced by pumping action of the donor. This is further helped by the stickiness of the stromal interfaces which may contribute to fixation of the transplant. The advantages of leaving patients anterior cornea intact are obvious as listed in Table 1.
Table 1: Advantages of endothelial keratoplasty (DSEK / DSAEK)
1. Reduced postoperative astigmatism.
2. Stable tear film
3. Early visual rehabilitation
4. No epithelial and stromal rejection
5. No postoperative suture-loosening and infections.
Donor preparation:
The method for harvesting the endothelium is a meticulous process. The donor cornea with is placed on an artificial chamber and lamellar dissection is done at the depth of 350 microns with specially designed instruments. Use of an automated technique like a microkeratome has decreased the failure rates of donor preparation.
Artificial Anterior Chamber (AAC, Figure 1) linked to the Amadeus II microkeratome is an excellent tool to obtain the posterior donor lamella for DSAEK. Advantages of donor preparation with micro-keratome are listed in Table 2. At present, microkeratome assisted DSAEK remains the procedure of choice for endothelial disorders of cornea.
Figure 1: Amadeus microkeratome assembled with artificial anterior chamber (AAC)
Table 2: Advantages of automated (microkeratome assisted) donor preparation:
1. Predictable donor thickness
2. Faster, less traumatic
3. Less interface haze
4. Better visual outcome.
DSAEK technique:
A small corneal incision is made and recipient’s damaged endothelial cells are removed. The harvested donor tissue is then inserted into the recipient eye. Different techniques have been described for the graft insertion which include folding method, push in technique and more recent pull-in technique using a specially designed inserter (Busin glide) along with endothelial grasping forceps.
Busin glide and endothelial grasping forceps are 2 critical instruments required in DSAEK. Busin glide (Figure 2) is used to atraumatically insert the endothelial tissue through a clear corneal incision. It has a platform for placement of endothelial tissue and a funnel-shaped tapering tip which is apposed at the corneal incision to allow insertion of the endothelial tissue with the assistance of an ‘endothelial grasping forceps’ (Figure 3). This 23-gauge micro-incision end-grasping forceps gently grasps the edge of the endothelial tissue to facilitate the ‘pull through’ technique.
Figure 2: Busin glide
Figure 3: Endothelial grasping forceps
The donor lenticule is then secured at its position by an air bubble injected through a small incision. The pull-in technique is summarized in Figure 4.
Figure 4: Pull-in technique
DSAEK results:
We have been performing DSEK procedure in Shroff Eye Centre for the last 3 years and have moved on to automated donor dissection with Amadeus II micro-keratome with a 450 micron head. Now, with Busin glide and endothelial grasping forceps, the DSAEK procedure has become even more predictable and less traumatic.
DSAEK procedure provides best results when there is no stromal opacity and ocular surface is healthy (Figure 5). However, many patients with a longstanding endothelial disease develop superficial corneal scarring and vascularization due to recurrent episodes of infections. We have found that a combining specialized additional procedures like superficial keratectomy at the time of DSAEK procedure removes most of the superficial scarring provides gratifying visual outcomes (Figure 6). Later on, these patients can be treated with laser to further improve the vision.
To conclude, DSAEK not only provides a lower induced astigmatism and faster visual recovery but also reduces the risks of graft failures associated with a conventional full thickness corneal transplant.
Legends to figures:
Figure 5: DSEK. Fig 5a. A clear DSEK graft in a patient with Psedophakic bullous keratopathy. Fig 5b. A well apposed posterior lenticule without any interface haze. Fig 5c. Pentacam Scheimpflug image showing the DSEK graft lenticule well apposed to the posterior surface of recipient cornea.
Know More...
 Dr. Rushad Shroff
Dr. Rushad Shroff Dr. Ritu Arora
Dr. Ritu Arora Dr. Dariel Mathur
Dr. Dariel Mathur Dr. Deepender Chauhan
Dr. Deepender Chauhan Dr. Amit Kumar Chawla
Dr. Amit Kumar Chawla Dr. Abhilasha Sanoria
Dr. Abhilasha Sanoria
 The cornea is the front transparent window of the eye. It is lamellar in nature (like plywood) and is made up of 5 layers, each of which has a definite function. In order to be effective it must remain transparent. Damage to any layers of cornea by degenerative change, infection, injury or scar tissue causes blurred vision due to loss of its transparency. Such a condition is called as corneal blindness.
The cornea is the front transparent window of the eye. It is lamellar in nature (like plywood) and is made up of 5 layers, each of which has a definite function. In order to be effective it must remain transparent. Damage to any layers of cornea by degenerative change, infection, injury or scar tissue causes blurred vision due to loss of its transparency. Such a condition is called as corneal blindness.







 Call Now
Call Now Book an
Book an Chat
Chat